Peripheral ischemia: what it is and how to control it
IMPORTANT: Peripheral ischemia, also called peripheral arterial disease of the lower limbs, is a serious, chronic, progressive disease that, in advanced forms, can lead to amputation. Diagnosis, monitoring, and treatment belong to the specialist (vascular surgeon, cardiologist, angiologist). Everything that follows is general information and adjunctive support. It does not replace antiplatelet medication, statin treatment, blood pressure and diabetes control, or the endovascular and surgical procedures recommended. Any herb, supplement, or change in regimen must be discussed with the attending physician.
Peripheral ischemia is, in a sense, the expression of a body that has grown tired of pushing blood through arteries narrowed by atheromatous plaque. The most common location is in the legs, where partially blocked arteries can no longer deliver enough blood during walking. The patient begins to feel pain in the calf when walking, a pain that disappears on stopping. This is the classic sign of intermittent claudication.
The disease does not appear overnight. It builds over years, on a background of the four major cardiovascular risk factors: smoking, diabetes, high blood pressure, and high cholesterol. Alongside them come age and family history. Peripheral ischemia is, essentially, atherosclerosis. The same plaques that close the leg arteries can close the heart or brain arteries as well. That is why a patient with peripheral arterial disease is automatically a patient with high cardiovascular risk.
The news many underestimate is that, treated in time, the disease can be held back for a long while. Modern medication, quitting smoking, supervised walking therapy, endovascular procedures, all of these give patients many more years of walking on their own feet. The secret is not to ignore the first signs.
Contents
- What peripheral ischemia is
- Causes and risk factors
- Signs and stages of the disease
- How the diagnosis is made
- Available medical treatments
- Walking therapy, the gold of the cure
- Anti-atherosclerotic nutrition
- Natural adjunctive support
- Practical tips
- Frequently asked questions
What peripheral ischemia is
Arteries are the conduits through which oxygenated blood is sent from the heart to the entire body. Over time, their inner wall can accumulate atheromatous plaques made of cholesterol, calcium, and inflammatory cells. These plaques narrow the artery and, in advanced stages, can almost completely block it. When this process occurs in the leg arteries (iliac, femoral, popliteal, tibial), we speak of peripheral arterial disease or peripheral ischemia.
Because walking requires a lot of oxygen in the calf muscles, the first manifestation appears here: a pain that forces the patient to stop after a short distance. At rest, the muscle gets enough oxygen and the pain fades. On starting again, pain returns at about the same distance. This phenomenon is called intermittent claudication.
How it differs from other walking pains
- Osteoarthritis pain changes with movement but does not fully disappear on stopping
- Neurological pain (disc herniation, spinal stenosis) has a different pattern and other symptoms
- Venous pain is diffuse, feels heavy, appears by evening, and is not strictly linked to distance walked
- Ischemic pain appears at a fairly constant distance and disappears only on stopping
Causes and risk factors
In 90% of cases, peripheral ischemia is a consequence of atherosclerosis. The rest come from rarer causes: Buerger’s disease in young smokers, vasculitis, thromboembolism, external compression.
Major risk factors
- Smoking, by far the strongest factor
- Diabetes mellitus, especially type 2
- High blood pressure
- High LDL cholesterol
- Obesity
- Sedentary lifestyle
- Age above 55
- Family history of cardiovascular disease
- Male sex, although women reach similar risk after menopause
- Chronic kidney disease
- Chronic stress
In diabetic patients, ischemia is frequently associated with peripheral neuropathy, and the diabetic foot becomes a separate topic because it suffers at three levels: vessel, nerve, and skin.
Signs and stages of the disease
The Fontaine classification divides peripheral arterial disease into four stages.
Stage I: asymptomatic
The patient has no pain, but arteries already show plaques. It is discovered accidentally, on Doppler ultrasound or measurement of the ankle-brachial index.
Stage II: intermittent claudication
The classic stage. The patient walks a certain distance, then pain appears in the calf, more rarely in the thigh or buttock. They stop, pain fades, they start again. It is split into IIa (more than 200 m without pain) and IIb (less than 200 m).
Stage III: rest pain
Pain appears even without effort, especially at night. The patient sleeps with the leg hanging off the bed, because gravity helps circulation slightly. This is already an advanced stage.
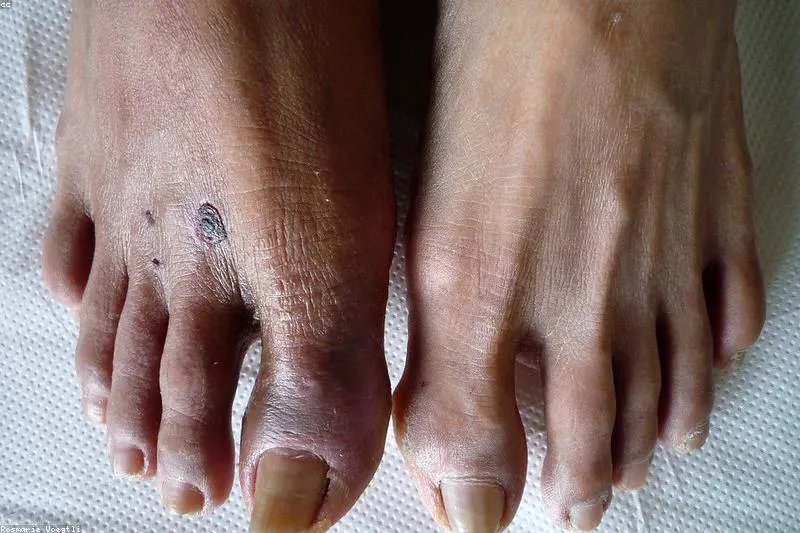
Stage IV: trophic lesions
Ulcerations and necrosis appear. Typical areas are the toes, heel, and front of the tibia. Any patient with non-healing wounds should be urgently evaluated vascularly.
Additional signs
- Foot paleness when the leg is elevated
- Intense redness when the leg is lowered
- Thin, shiny skin
- Hair loss on the calf
- Brittle, thick, yellow nails
- Cold skin to the touch
- Absent pulse at the posterior tibial or dorsalis pedis arteries
How the diagnosis is made
The doctor palpates pulses and measures the ankle-brachial index (ABI). It is a simple, painless test that compares ankle pressure with arm pressure. A value below 0.9 confirms peripheral arterial disease.
Basic investigations
- Ankle-brachial index
- Arterial Doppler ultrasound of the lower limbs
- Treadmill walking test, sometimes
- Blood tests (glucose, cholesterol, lipid profile, kidney function)
Advanced investigations
- CT angiography with contrast
- MR angiography
- Arteriography, usually with therapeutic intent
A patient with peripheral arterial disease is at high risk for heart attack and stroke, so investigations are also performed for the other territories: echocardiography, carotid ultrasound, stress test.
Available medical treatments
Treatment has three goals: reducing global cardiovascular risk, improving walking symptoms, preventing limb loss.
Drug treatment
- Antiplatelet agents (aspirin, clopidogrel)
- Statins, to lower cholesterol and stabilize plaques
- Blood pressure medications (ACE inhibitors, angiotensin receptor blockers)
- Diabetes treatment, with stricter targets than for other patients
- Cilostazol, a specific drug that increases walking distance
- Pentoxifylline, in selected cases
Procedures and surgery
- Balloon angioplasty, endovascular, with or without stent
- Arterial bypass, for long or multiple obstructions
- Endarterectomy, especially of the common femoral artery
- Amputation, the last option, when the limb cannot be saved
Smoking cessation
Quite simply, it is the most important measure in a patient who smokes. No drug has the effect of quitting cigarettes. There is counseling, medication for nicotine dependence, and replacement therapy. The doctor can guide the patient.
Walking therapy, the gold of the cure
There is a recommendation that seems paradoxical: the patient with walking pain is advised to walk. But not any way. Supervised walking therapy is one of the most powerful treatments in stage II of the disease.
How it is done
- At least three sessions a week
- 30-60 minutes per session
- Walk until moderate, not unbearable, pain appears
- Pause until pain subsides
- Resume walking
- Repeat the cycle through the whole session
Over time, pain-free distance increases. Collateral circulation develops, muscles become more energy-efficient, metabolism improves. The effect is comparable, in some cases, to interventional procedures.
The ideal is supervised walking in specialized centers, but home walking, respecting the rules, brings substantial benefits too.
Anti-atherosclerotic nutrition
Peripheral arterial disease is an expression of atherosclerosis, and nutrition matters a lot.
What is recommended
- Mediterranean diet with fruits, vegetables, whole grains, extra virgin olive oil, fatty fish
- Fiber from legumes, oats, seeds
- Nuts and seeds (walnuts, almonds, pistachios) for cardioprotective effect
- Fatty fish 2-3 times a week
- Garlic and onion, for positive effects on cholesterol and blood pressure
- Red and purple fruits, rich in antioxidants
What to limit
- Processed meat (sausages, ham, salami, cold cuts)
- Trans fats (old margarines, ultra-processed products)
- Large amounts of refined sugar
- Excess salt
- Alcohol beyond moderate limits
- Repeated deep frying
Natural adjunctive support
Several herbs and supplements have studies suggesting beneficial effects. But none replace prescribed medication.
Studied herbs
- Ginkgo biloba, for microcirculation, in some studies has shown modest gains in walking distance
- Garlic, with mild effects on blood pressure and cholesterol
- Hawthorn, traditionally used for cardiac support
- Turmeric, for systemic anti-inflammatory effect
- Omega 3 from fish oil, for the lipid profile
- Coenzyme Q10, especially in patients on statins, for muscle discomfort
Drug interactions are real. Ginkgo, for example, can increase bleeding risk in patients on aspirin. So any addition must be discussed with the doctor.
Teas that support circulation
- Hawthorn tea, 1-2 cups a day
- Green tea, for antioxidants
- Ginger tea, for general tonic effect
- Nettle tea, mild diuretic, rich in iron
Practical tips
- Quit smoking, today, not tomorrow
- Measure your blood pressure regularly
- Monitor blood sugar if you have diabetes or prediabetes
- Check your lipid profile annually
- Walk daily, following walking therapy rules
- Protect your feet, avoid injuries (overgrown nails, uncomfortable shoes)
- Inspect the sole and toes daily, look for wounds
- Wash feet with lukewarm water, dry well between toes
- Moisturize skin to prevent cracking
- Do not go barefoot, especially if you have diabetes
- Wear wide, round-toed shoes
- See the doctor urgently if non-healing wounds appear
Frequently asked questions
Can peripheral ischemia be cured? It cannot be cured in the sense of disappearing completely, but it can be controlled effectively, sometimes very well. The goal is to stop progression and improve quality of life.
Doesn’t walking hurt if it causes pain? No, on the contrary. The patient is encouraged to walk until moderate pain appears, stop until it subsides, then continue. This cycle stimulates collateral circulation to form.
If I have been operated on the arteries, do I still need medication? Yes. The procedure does not cure atherosclerosis. Medication and lifestyle are lifelong.
Is a cold foot always a sign of ischemia? Not necessarily. A cold foot can appear due to Raynaud’s syndrome, from cold weather, or vasoconstrictive reflexes. But if it is associated with pain, pallor, and absent pulse, ischemia must be evaluated.
Can I do intense sports with peripheral arterial disease? Yes, with medical approval. Walking, swimming, and cycling are preferable. High-impact sports are discussed individually.
Can I use ginkgo biloba alongside aspirin? Only with the doctor’s approval. The combination may increase bleeding risk, especially if you are also on other antiplatelet agents.
What is the best shoe for a patient with ischemia? A wide shoe with a flexible sole, round toe, and no hard inner seams. Check the inside before each use to make sure there is no small stone or folded sock.
Peripheral ischemia is a disease marked by daily decisions. More than many others, it gets better or worse depending on what you choose: smoking or quitting, walking or sitting, eating well or not. If you get to serious work on all axes and partner closely with your vascular doctor, you can enjoy free walking for many years. If you drift, complications settle in. Choose wisely, choose in time.
